Types of Addictive Substances
|
|
Drug abuse is a serious public health problem that affects almost every community and family in some way. Each year drug abuse results in around 40 million serious illnesses or injuries among people in the United States. Abused drugs include:
Make sure to download and review this table. It provides important information about substance categories, use methods, and consequences.
|
| ||||||
Drug abuse also plays a role in many major social problems, such as drugged driving, violence, stress, and child abuse. Drug abuse can lead to homelessness, crime and missed work or problems with keeping a job. There are different types of treatment for drug abuse. But the best is to prevent drug abuse in the first place.
Club Drugs
|
The term club drug refers to a wide variety of dangerous drugs. These drugs are often used by young adults at all-night dance parties, dance clubs and bars. They include
Club drugs have become more common in recent years. Sometimes people use them to commit sexual assaults. Club drugs can cause serious health problems and sometimes death. They are even more dangerous if you use them with alcohol. |
How Do Club Drugs Affect the Brain?
Addictive Potential
Repeated use of GHB may lead to withdrawal effects, including insomnia, anxiety, tremors, and sweating. Severe withdrawal reactions have been reported among patients presenting from an overdose of GHB or related compounds, especially if other drugs or alcohol are involved.
What Other Adverse Effects Do Club Drugs Have on Health?
Uncertainties about the sources, chemicals, and possible contaminants used to manufacture many club drugs make it extremely difficult to determine toxicity and associated medical consequences. Nonetheless, we do know that:
- At high doses, GHB’s sedative effects may result in sleep, coma, or death.
- Rohypnol can produce anterograde amnesia, in which individuals may not remember events they experienced while under the influence of the drug.
- Ketamine is a dissociative anesthetic, so called because it distorts perceptions of sight and sound and produces feelings of detachment from the environment and self. Low-dose intoxication results in impaired attention, learning ability, and memory. At higher doses, ketamine can cause dreamlike states and hallucinations; and at higher doses still, ketamine can cause delirium and amnesia.
Addictive Potential
Repeated use of GHB may lead to withdrawal effects, including insomnia, anxiety, tremors, and sweating. Severe withdrawal reactions have been reported among patients presenting from an overdose of GHB or related compounds, especially if other drugs or alcohol are involved.
- Like other benzodiazepines, chronic use of Rohypnol can produce tolerance, physical dependence, and addiction.
- There have been reports of people binging on ketamine, a behavior that is similar to that seen in some cocaine- or amphetamine-dependent individuals. Ketamine users can develop signs of tolerance and cravings for the drug.
What Other Adverse Effects Do Club Drugs Have on Health?
Uncertainties about the sources, chemicals, and possible contaminants used to manufacture many club drugs make it extremely difficult to determine toxicity and associated medical consequences. Nonetheless, we do know that:
- Coma and seizures can occur following use of GHB. Combined use with other drugs such as alcohol can result in nausea and breathing difficulties. GHB has been involved in poisonings, overdoses, date rapes, and deaths.
- Rohypnol may be lethal when mixed with alcohol and/or other CNS depressants.
- Ketamine, in high doses, can cause impaired motor function, high blood pressure, and potentially fatal respiratory problems.
Methamphetamine
|
Methamphetamine is a very addictive stimulant drug. It can be smoked, injected, inhaled or taken by mouth. It has many street names, such as speed, meth, and chalk. Methamphetamine hydrochloride, the crystal form inhaled by smoking, is referred to as ice, crystal, glass and Tina. Methamphetamine affects the brain and can create feelings of pleasure, increase energy and elevate mood. Abusers may become addicted quickly, needing higher doses more often. Adverse health effects include irregular heartbeat, increased blood pressure and a variety of psychological problems. Long-term effects may include severe mental disorders, memory loss and severe dental problems.
|
How Does Methamphetamine Affect the Brain?
Methamphetamine increases the release and blocks the reuptake of the brain chemical (or neurotransmitter) dopamine, leading to high levels of the chemical in the brain—a common mechanism of action for most drugs of abuse. Dopamine is involved in reward, motivation, the experience of pleasure, and motor function. Methamphetamine’s ability to release dopamine rapidly in reward regions of the brain produces the intense euphoria, or “rush,” that many users feel after snorting, smoking, or injecting the drug.
Chronic methamphetamine abuse significantly changes how the brain functions. Noninvasive human brain imaging studies have shown alterations in the activity of the dopamine system that are associated with reduced motor skills and impaired verbal learning. Recent studies in chronic methamphetamine abusers have also revealed severe structural and functional changes in areas of the brain associated with emotion and memory, which may account for many of the emotional and cognitive problems observed in chronic methamphetamine abusers.
Repeated methamphetamine abuse can also lead to addiction—a chronic, relapsing disease characterized by compulsive drug seeking and use, which is accompanied by chemical and molecular changes in the brain. Some of these changes persist long after methamphetamine abuse is stopped. Reversal of some of the changes, however, may be observed after sustained periods of abstinence (e.g., more than 1 year).
What Other Adverse Effects Does Methamphetamine Have on Health?
Taking even small amounts of methamphetamine can result in many of the same physical effects as those of other stimulants, such as cocaine or amphetamines, including increased wakefulness, increased physical activity, decreased appetite, increased respiration, rapid heart rate, irregular heartbeat, increased blood pressure, and hyperthermia.
Long-term methamphetamine abuse has many negative health consequences, including
extreme weight loss, severe dental problems (“meth mouth”), anxiety, confusion, insomnia, mood disturbances, and violent behavior. Chronic methamphetamine abusers can also display a number of psychotic features, including paranoia, visual and auditory hallucinations, and delusions (for example, the sensation of insects crawling under the skin).
Transmission of HIV and hepatitis B and C can be consequences of methamphetamine abuse. The intoxicating effects of methamphetamine, regardless of how it is taken, can also alter judgment and inhibition and can lead people to engage in unsafe behaviors, including risky sexual behavior. Among abusers who inject the drug, HIV/AIDS and other infectious diseases can be spread through contaminated needles, syringes, and other injection equipment that is used by more than one person. Methamphetamine abuse may also worsen the progression of HIV/AIDS and its consequences. Studies of methamphetamine abusers who are HIV-positive indicate that HIV causes greater neuronal injury and cognitive impairment for individuals in this group compared with HIV-positive people who do not use the drug.
|
Anabolic Steroids
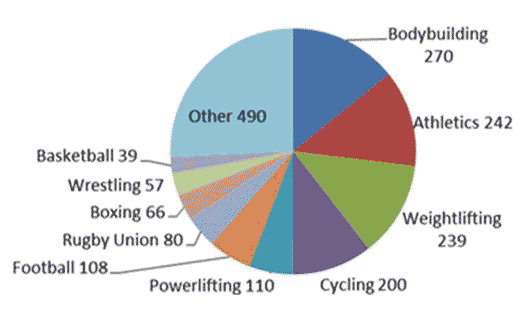
Anabolic-androgenic steroids (AAS) are synthetically produced variants of the naturally occurring male sex hormone testosterone. “Anabolic” refers to muscle-building, and “androgenic” refers to increased male sexual characteristics. “Steroids” refers to the class of drugs. These drugs can be legally prescribed to treat conditions resulting from steroid hormone deficiency, such as delayed puberty, as well as diseases that result in loss of lean muscle mass, such as cancer and AIDS.
|
How Do AAS Affect the Brain?
The acute effects of AAS in the brain are substantially different from those of other drugs of abuse. The most important difference is that AAS are not euphorigenic, meaning they do not trigger rapid increases in the neurotransmitter dopamine, which is responsible for the “high” that often drives substance abuse behaviors. However, long-term use of AAS can eventually have an impact on some of the same brain pathways and chemicals—such as dopamine, serotonin, and opioid systems—that are affected by other drugs of abuse. Considering the combined effect of their complex direct and indirect actions, it is not surprising that AAS can affect mood and behavior in significant ways.
AAS and Mental Health
Preclinical, clinical, and anecdotal reports suggest that steroids may contribute to psychiatric dysfunction. Research shows that abuse of anabolic steroids may lead to aggression and other adverse effects. For example, although many users report feeling good about themselves while on anabolic steroids, extreme mood swings can also occur, including manic-like symptoms that could lead to violence. Researchers have also observed that users may suffer from paranoid jealousy, extreme irritability, delusions, and impaired judgment stemming from feelings of invincibility.
Addictive Potential
Animal studies have shown that AAS are reinforcing—that is, animals will self-administer AAS when given the opportunity, just as they do with other addictive drugs. This property is more difficult to demonstrate in humans, but the potential for AAS abusers to become addicted is consistent with their continued abuse despite physical problems and negative effects on social relations. Also, steroid abusers typically spend large amounts of time and money obtaining the drug: this is another indication of addiction. Individuals who abuse steroids can experience withdrawal symptoms when they stop taking AAS—these include mood swings, fatigue, restlessness, loss of appetite, insomnia, reduced sex drive, and steroid cravings, all of which may contribute to continued abuse. One of the most dangerous withdrawal symptoms is depression— when persistent, it can sometimes lead to suicide attempts.
Research also indicates that some users might turn to other drugs to alleviate some of the negative effects of AAS. For example, a study of 227 men admitted in 1999 to a private treatment center for dependence on heroin or other opioids found that 9.3 percent had abused AAS before trying any other illicit drug. Of these, 86 percent first used opioids to counteract insomnia and irritability resulting from the steroids.
What Other Adverse Effects Do AAS Have on Health?
Steroid abuse can lead to serious, even irreversible health problems. Some of the most dangerous among these include liver damage; jaundice (yellowish pigmentation of skin, tissues, and body fluids); fluid retention; high blood pressure; increases in LDL (“bad” cholesterol); and decreases in HDL (“good” cholesterol). Other reported effects include renal failure, severe acne, and trembling. In addition, there are some gender- and age- specific adverse effects:
- For men—shrinking of the testicles, reduced sperm count, infertility, baldness, development of breasts, increased risk for prostate cancer
- For women—growth of facial hair, male-pattern baldness, changes in or cessation of the menstrual cycle, enlargement of the clitoris, deepened voice
- For adolescents—stunted growth due to premature skeletal maturation and accelerated puberty changes; risk of not reaching expected height if AAS is taken before the typical adolescent growth spurt
Cocaine
|
Cocaine is a powerful drug that stimulates the brain. People who use it can form a strong addiction. They may have to use more and more of the drug to get high. It's sold on the street as a fine, white powder. There are two forms of cocaine: hydrochloride salt and freebase. The salt dissolves in water. People can take it in a vein or in the nose. The freebase form can be smoked. Crack is the street name of a smokable form of cocaine. No matter how cocaine is taken, it is dangerous. Some of the most common serious problems include
|
- Heart problems, including heart attacks
- Respiratory effects, including respiratory failure
- Nervous system problems, including strokes
- Digestive problems
How Does Cocaine Affect the Brain?
Cocaine is a strong central nervous system stimulant that increases levels of dopamine, a brain chemical (or neurotransmitter) associated with pleasure and movement, in the brain’s reward circuit. Certain brain cells, or neurons, use dopamine to communicate. Normally, dopamine is released by a neuron in response to a pleasurable signal (e.g., the smell of good food), and then recycled back into the cell that released it, thus shutting off the signal between neurons.
Cocaine acts by preventing the dopamine from being recycled, causing excessive amounts of the neurotransmitter to build up, amplifying the message to and response of the receiving neuron, and ultimately disrupting normal communication. It is this excess of dopamine that is responsible for cocaine’s euphoric effects. With repeated use, cocaine can cause long-term changes in the brain’s reward system and in other brain systems as well, which may eventually lead to addiction. With repeated use, tolerance to the cocaine high also often develops. Many cocaine abusers report that they seek but fail to achieve as much pleasure as they did from their first exposure. Some users will increase their dose in an attempt to intensify and prolong the euphoria, but this can also increase the risk of adverse psychological or physiological effects.
What Adverse Effects Does Cocaine Have on Health?
Abusing cocaine has a variety of adverse effects on the body. For example, cocaine constricts blood vessels, dilates pupils, and increases body temperature, heart rate, and blood pressure. It can also cause headaches and gastrointestinal complications such as abdominal pain and nausea. Because cocaine tends to decrease appetite, chronic users can become malnourished as well.
Different methods of taking cocaine can produce different adverse effects. Regular intranasal use (snorting) of cocaine, for example, can lead to loss of the sense of smell; nosebleeds; problems with swallowing; hoarseness; and a chronically runny nose.
Ingesting cocaine can cause severe bowel gangrene as a result of reduced blood flow. Injecting cocaine can bring about severe allergic reactions and increased risk for contracting HIV/AIDS and other blood-borne diseases. Binge-patterned cocaine use may lead to irritability, restlessness, and anxiety. Cocaine abusers can also experience severe paranoia—a temporary state of full-blown paranoid psychosis—in which they lose touch with reality and experience auditory hallucinations. Regardless of the route or frequency of use, cocaine abusers can experience acute cardiovascular or cerebrovascular emergencies, such as a heart attack or stroke, which may cause sudden death. Cocaine-related deaths are often a result of cardiac arrest or seizure followed by respiratory arrest.
Heroin
|
Heroin is a drug made from morphine, a natural substance in the seedpod of the Asian poppy plant. Heroin usually appears as a white or brown powder. Heroin can be injected, smoked or snorted. Heroin abuse is a serious problem in the United States. Major health problems from heroin include miscarriages, heart infections and death from overdose.
People who inject the drug also risk infectious diseases, including HIV/AIDS and hepatitis. Regular use of heroin can lead to tolerance. This means users need more and more drug to have the same effect. At higher doses over time, the body becomes dependent on heroin. If dependent users stop heroin, they have withdrawal symptoms. These symptoms include restlessness, muscle and bone pain, diarrhea, vomiting and cold flashes. |
How Does Heroin Affect the Brain?
Heroin enters the brain, where it is converted to morphine and binds to receptors known as opioid receptors. These receptors are located in many areas of the brain (and in the body), especially those involved in the perception of pain and in reward. Opioid receptors are also located in the brain stem—important for automatic processes critical for life, such as breathing (respiration), blood pressure, and arousal. Heroin overdoses frequently involve a suppression of respiration.
After an intravenous injection of heroin, users report feeling a surge of euphoria (“rush”) accompanied by dry mouth, a warm flushing of the skin, heaviness of the extremities, and clouded mental functioning. Following this initial euphoria, the user goes “on the nod,” an alternately wakeful and drowsy state. Users who do not inject the drug may not experience the initial rush, but other effects are the same.
With regular heroin use, tolerance develops, in which the user’s physiological (and psychological) response to the drug decreases, and more heroin is needed to achieve the same intensity of effect. Heroin users are at high risk for addiction—it is estimated that about 23 percent of individuals who use heroin become dependent on it.
What Other Adverse Effects Does Heroin Have on Health?
Heroin abuse is associated with serious health conditions, including fatal overdose, spontaneous abortion, and—particularly in users who inject the drug—infectious diseases, including HIV/AIDS and hepatitis. Chronic users may develop collapsed veins, infection of the heart lining and valves, abscesses, and liver or kidney disease. Pulmonary complications, including various types of pneumonia, may result from the poor health of the abuser as well as from heroin’s depressing effects on respiration. In addition to the effects of the drug itself, street heroin often contains toxic contaminants or additives that can clog blood vessels leading to the lungs, liver, kidneys, or brain, causing permanent damage to vital organs.
Chronic use of heroin leads to physical dependence, a state in which the body has adapted to the presence of the drug. If a dependent user reduces or stops use of the drug abruptly, he or she may experience severe symptoms of withdrawal. These symptoms—which can begin as early as a few hours after the last drug administration—can include restlessness, muscle and bone pain, insomnia, diarrhea and vomiting, cold flashes with goose bumps (“cold turkey”), and kicking movements (“kicking the habit”). Users also experience severe craving for the drug during withdrawal, which can precipitate continued abuse and/or relapse.
Major withdrawal symptoms peak between 48 and 72 hours after the last dose of the drug and typically subside after about 1 week. Some individuals, however, may show persistent withdrawal symptoms for months. Although heroin withdrawal is considered less dangerous than alcohol or barbiturate withdrawal, sudden withdrawal by heavily dependent users who are in poor health is occasionally fatal. In addition, heroin craving can persist years after drug cessation, particularly upon exposure to triggers such as stress or people, places, and things associated with drug use.
Heroin abuse during pregnancy, together with related factors like poor nutrition and inadequate prenatal care, has been associated with adverse consequences including low birthweight, an important risk factor for later developmental delay. If the mother is regularly abusing the drug, the infant may be born physically dependent on heroin and could suffer from serious medical complications requiring hospitalization.
Heroin enters the brain, where it is converted to morphine and binds to receptors known as opioid receptors. These receptors are located in many areas of the brain (and in the body), especially those involved in the perception of pain and in reward. Opioid receptors are also located in the brain stem—important for automatic processes critical for life, such as breathing (respiration), blood pressure, and arousal. Heroin overdoses frequently involve a suppression of respiration.
After an intravenous injection of heroin, users report feeling a surge of euphoria (“rush”) accompanied by dry mouth, a warm flushing of the skin, heaviness of the extremities, and clouded mental functioning. Following this initial euphoria, the user goes “on the nod,” an alternately wakeful and drowsy state. Users who do not inject the drug may not experience the initial rush, but other effects are the same.
With regular heroin use, tolerance develops, in which the user’s physiological (and psychological) response to the drug decreases, and more heroin is needed to achieve the same intensity of effect. Heroin users are at high risk for addiction—it is estimated that about 23 percent of individuals who use heroin become dependent on it.
What Other Adverse Effects Does Heroin Have on Health?
Heroin abuse is associated with serious health conditions, including fatal overdose, spontaneous abortion, and—particularly in users who inject the drug—infectious diseases, including HIV/AIDS and hepatitis. Chronic users may develop collapsed veins, infection of the heart lining and valves, abscesses, and liver or kidney disease. Pulmonary complications, including various types of pneumonia, may result from the poor health of the abuser as well as from heroin’s depressing effects on respiration. In addition to the effects of the drug itself, street heroin often contains toxic contaminants or additives that can clog blood vessels leading to the lungs, liver, kidneys, or brain, causing permanent damage to vital organs.
Chronic use of heroin leads to physical dependence, a state in which the body has adapted to the presence of the drug. If a dependent user reduces or stops use of the drug abruptly, he or she may experience severe symptoms of withdrawal. These symptoms—which can begin as early as a few hours after the last drug administration—can include restlessness, muscle and bone pain, insomnia, diarrhea and vomiting, cold flashes with goose bumps (“cold turkey”), and kicking movements (“kicking the habit”). Users also experience severe craving for the drug during withdrawal, which can precipitate continued abuse and/or relapse.
Major withdrawal symptoms peak between 48 and 72 hours after the last dose of the drug and typically subside after about 1 week. Some individuals, however, may show persistent withdrawal symptoms for months. Although heroin withdrawal is considered less dangerous than alcohol or barbiturate withdrawal, sudden withdrawal by heavily dependent users who are in poor health is occasionally fatal. In addition, heroin craving can persist years after drug cessation, particularly upon exposure to triggers such as stress or people, places, and things associated with drug use.
Heroin abuse during pregnancy, together with related factors like poor nutrition and inadequate prenatal care, has been associated with adverse consequences including low birthweight, an important risk factor for later developmental delay. If the mother is regularly abusing the drug, the infant may be born physically dependent on heroin and could suffer from serious medical complications requiring hospitalization.
|
Pay special attention to Slide Five. If the file does not load below, please visit it here.
|
Marijuana
Marijuana
|
Marijuana is the most commonly abused illicit drug in the United States. It is a dry, shredded green and brown mix of flowers, stems, seeds, and leaves derived from the hemp plant Cannabis sativa. The main active chemical in marijuana is delta-9- tetrahydrocannabinol, or THC for short.
How Does Marijuana Affect the Brain? Scientists have learned a great deal about how THC acts in the brain to produce its many effects. When someone smokes marijuana, THC rapidly passes from the lungs into the bloodstream, which carries the chemical to the brain and other organs throughout the body. THC acts upon specific sites in the brain, called cannabinoid receptors, kicking off a series of cellular reactions that ultimately lead to the "high" that users experience when they smoke marijuana. Some brain areas have many cannabinoid receptors; others have few or none. The highest density of cannabinoid receptors are found in parts of the brain that influence pleasure, memory, thinking, concentrating, sensory and time perception, and coordinated movement. |
Not surprisingly, marijuana intoxication can cause distorted perceptions, impaired coordination, difficulty with thinking and problem solving, and problems with learning and memory. Research has shown that, in chronic users, marijuana's adverse impact on learning and memory can last for days or weeks after the acute effects of the drug wear off. As a result, someone who smokes marijuana every day may be functioning at a suboptimal intellectual level all of the time.
Research into the effects of long-term cannabis use on the structure of the brain has yielded inconsistent results. It may be that the effects are too subtle for reliable detection by current techniques. A similar challenge arises in studies of the effects of chronic marijuana use on brain function. Brain imaging studies in chronic users tend to show some consistent alterations, but their connection to impaired cognitive functioning is far from clear. This uncertainty may stem from confounding factors such as other drug use, residual drug effects, or withdrawal symptoms in long-term chronic users.
What Other Adverse Effect Does Marijuana Have on Health?
Is Marijuana Medicine?
The potential medicinal properties of marijuana have been the subject of substantive research and heated debate. Scientists have confirmed that the cannabis plant contains active ingredients with therapeutic potential for relieving pain, controlling nausea, stimulating appetite, and decreasing ocular pressure. Cannabinoid-based medications include synthetic compounds, such as dronabinol (Marinol®) and nabilone (Cesamet®), which are FDA approved, and a new, chemically pure mixture of plant-derived THC and cannabidiol called Sativex®, formulated as a mouth spray and approved in Canada and parts of Europe for the relief of cancer-associated pain and spasticity and neuropathic pain in multiple sclerosis.
Scientists continue to investigate the medicinal properties of THC and other cannabinoids to better evaluate and harness their ability to help patients suffering from a broad range of conditions, while avoiding the adverse effects of smoked marijuana.
Research into the effects of long-term cannabis use on the structure of the brain has yielded inconsistent results. It may be that the effects are too subtle for reliable detection by current techniques. A similar challenge arises in studies of the effects of chronic marijuana use on brain function. Brain imaging studies in chronic users tend to show some consistent alterations, but their connection to impaired cognitive functioning is far from clear. This uncertainty may stem from confounding factors such as other drug use, residual drug effects, or withdrawal symptoms in long-term chronic users.
What Other Adverse Effect Does Marijuana Have on Health?
- Effects on the Heart: Marijuana increases heart rate by 20-100 percent shortly after smoking; this effect can last up to 3 hours. In one study, it was estimated that marijuana users have a 4.8-fold increase in the risk of heart attack in the first hour after smoking the drug. This may be due to increased heart rate as well as the effects of marijuana on heart rhythms, causing palpitations and arrhythmias. This risk may be greater in aging populations or in those with cardiac vulnerabilities.
- Effects on the Lungs: Marijuana users usually inhale more deeply and hold their breath longer than tobacco smokers do, which further increase the lungs' exposure to carcinogenic smoke. Marijuana smokers show dysregulated growth of epithelial cells in their lung tissue, which could lead to cancer; however, a recent case-controlled study found no positive associations between marijuana use and lung, upper respiratory, or upper digestive tract cancers. Thus, the link between marijuana smoking and these cancers remains unsubstantiated at this time.
- Nonetheless, marijuana smokers can have many of the same respiratory problems as tobacco smokers, such as daily cough and phlegm production, more frequent acute chest illness, and a heightened risk of lung infections. Many of the extra sick days among the marijuana smokers in the study were for respiratory illnesses.
Is Marijuana Medicine?
The potential medicinal properties of marijuana have been the subject of substantive research and heated debate. Scientists have confirmed that the cannabis plant contains active ingredients with therapeutic potential for relieving pain, controlling nausea, stimulating appetite, and decreasing ocular pressure. Cannabinoid-based medications include synthetic compounds, such as dronabinol (Marinol®) and nabilone (Cesamet®), which are FDA approved, and a new, chemically pure mixture of plant-derived THC and cannabidiol called Sativex®, formulated as a mouth spray and approved in Canada and parts of Europe for the relief of cancer-associated pain and spasticity and neuropathic pain in multiple sclerosis.
Scientists continue to investigate the medicinal properties of THC and other cannabinoids to better evaluate and harness their ability to help patients suffering from a broad range of conditions, while avoiding the adverse effects of smoked marijuana.
Prescription Drugs
Most people take medicines only for the reasons their doctors prescribe them. But an estimated 20 percent of people in the United States have used prescription drugs for non-medical reasons. This is prescription drug abuse. It is a serious and growing problem. Abusing some prescription drugs can lead to addiction. You can develop an addiction to:
Experts do not know exactly why this type of drug abuse is increasing. The availability of drugs is probably one reason. Doctors are prescribing more drugs for more health problems than ever before. Online pharmacies make it easy to get prescription drugs without a prescription, even for younger people.
Commonly Abused Prescription Drugs
Medications can be effective when they are used properly, but some can be addictive and dangerous when abused. Some prescribed medications that - when used in ways or by people other than prescribed - have the potential for adverse medical consequences, including addiction. In 2010, approximately 16 million Americans reported using a prescription drug for non-medical reasons in the past year; 7 million in the past month. After marijuana, prescription and over-the-counter medications account for most of the commonly abused drugs.
What types of prescription drugs are abused?
Three types of drugs are abused most often:
Prescription Drug Advertising
Your healthcare provider is the best source of information about the right medicines for you. The Food and Drug Administration (FDA) protects public health by assuring the safety, effectiveness, and security of a wide range of products, including human prescription drugs. We also advance public health by helping people get the accurate, science-based information they need to use medicines appropriately and improve their health. Prescription drug advertisements can provide useful information for consumers to work with their health care providers to make wise decisions about treatment.
- Narcotic painkillers
- Sedatives and tranquilizers
- Stimulants
Experts do not know exactly why this type of drug abuse is increasing. The availability of drugs is probably one reason. Doctors are prescribing more drugs for more health problems than ever before. Online pharmacies make it easy to get prescription drugs without a prescription, even for younger people.
Commonly Abused Prescription Drugs
Medications can be effective when they are used properly, but some can be addictive and dangerous when abused. Some prescribed medications that - when used in ways or by people other than prescribed - have the potential for adverse medical consequences, including addiction. In 2010, approximately 16 million Americans reported using a prescription drug for non-medical reasons in the past year; 7 million in the past month. After marijuana, prescription and over-the-counter medications account for most of the commonly abused drugs.
What types of prescription drugs are abused?
Three types of drugs are abused most often:
- Opioids—prescribed for pain relief
- CNS depressants—barbiturates and benzodiazepines prescribed for anxiety or sleep problems (often referred to as sedatives or tranquilizers)
- Stimulants—prescribed for attention-deficit hyperactivity disorder (ADHD), the sleep disorder narcolepsy, or obesity.
Prescription Drug Advertising
Your healthcare provider is the best source of information about the right medicines for you. The Food and Drug Administration (FDA) protects public health by assuring the safety, effectiveness, and security of a wide range of products, including human prescription drugs. We also advance public health by helping people get the accurate, science-based information they need to use medicines appropriately and improve their health. Prescription drug advertisements can provide useful information for consumers to work with their health care providers to make wise decisions about treatment.
|
FDA Authority Over Advertising
The FDA serves the public health and welfare in many ways. One way is overseeing the approval and marketing of prescription drugs. It's authority is based on a number of federal laws, including the Federal Food, Drug, and Cosmetic Act. Among other areas, this law specifically addresses prescription drug advertising. This law requires that advertisements for prescription drugs be accurate and not misleading. Direct-to-consumer (DTC) advertising is a relatively new area of prescription drug promotion. No federal law has ever banned DTC advertising. Until the mid-1980s, drug companies gave information about prescription drugs only to doctors and pharmacists. When these professionals thought it appropriate, they gave that information to their patients. However, during the 1980s, some drug companies started to give the general public more direct access to this information through DTC ads. The law requires that product claim ads give a "fair balance" of information about drug risks as compared with information about drug benefits. This means that the content and presentation of a drug's most important risks must be reasonably similar to the content and presentation of its benefits. This does not mean that equal space must be given to risks and benefits in print ads, or equal time to risks and benefits in broadcast ads. The amount of time or space needed to present risk information will depend on the drug's risks and the way that both the benefits and risks are presented. Think about the following questions when you see an ad for a prescription drug. Vertical Divider
|
Prescription medication considerations
Vertical Divider
|
Harmful Interactions: Mixing Alcohol with Medicines
You have probably seen this warning on medicines. The danger is real. Mixing alcohol with certain medications can cause nausea and vomiting, headaches, drowsiness, fainting, or loss of coordination. It also can put you at risk for internal bleeding, heart problems, and difficulties in breathing. In addition to these dangers, alcohol can make a medication less effective or even useless, or it may make the medication harmful or toxic to your body. Some medicines that you might never have suspected can react with alcohol, including many medications which can be purchased “over-the-counter”—that is, without a prescription. Even some herbal remedies can have harmful effects when combined with alcohol.
Medicines may have many ingredients
Some medications—including many popular painkillers and cough, cold, and allergy remedies—contain more than one ingredient that can react with alcohol. Read the label on the medication bottle to find out exactly what ingredients a medicine contains. Ask your pharmacist if you have any questions about how alcohol might interact with a drug you are taking.
Some medicines contain alcohol
Certain medicines contain up to 10% alcohol. Cough syrup and laxatives may have some of the highest alcohol concentrations.
Alcohol affects women differently
Women, in general, have a higher risk for problems than men. When a woman drinks, the alcohol in her bloodstream typically reaches a higher level than a man’s even if both are drinking the same amount. This is because women’s bodies generally have less water than men’s bodies. Because alcohol mixes with body water, a given amount of alcohol is more concentrated in a woman’s body than in a man’s. As a result, women are more susceptible to alcohol-related damage to organs such as the liver.
Older people face greater risk
Older people are at particularly high risk for harmful alcohol– medication interactions. Aging slows the body’s ability to break down alcohol, so alcohol remains in a person’s system longer. Older people also are more likely to take a medication that interacts with alcohol—in fact, they often need to take more than one of these medications.
Remember…
Mixing alcohol and medicines puts you at risk for dangerous reactions. Protect yourself by avoiding alcohol if you are taking a medication and don’t know its effect. Timing is important- alcohol and medicines can interact harmfully even if they are not taken at the same time.To learn more about a medicine and whether it will interact with alcohol, talk to your pharmacist or other health care provider.
|
|
|
Alcohol Abuse
|
any people drink alcohol at least occasionally. For many people, moderate drinking is probably safe. It may even have health benefits, including reducing your risk of certain heart problems. Moderate drinking is one drink a day for women or anyone over 65, and two drinks a day for men under 65. Some people should not drink at all, including alcoholics, children, pregnant women, people on certain medicines and people with some medical conditions.
Anything more than moderate drinking can be risky. Binge drinking - drinking five or more drinks at one time - can damage your health and increase your risk for accidents, injuries and assault. Years of heavy drinking can lead to liver disease, heart disease, cancer and pancreatitis. It can also cause problems at home, at work and with friends. Quick Quiz
|
Quick Quiz Answers: 1) males-5 or more within a short period of time, females- 4 or more within a short period of time; 2) true; 3) Alcohol; 4) true
|
Beyond Hangovers
Alcohol is part of our culture—it helps us celebrate and socialize, and it enhances our religious ceremonies. But drinking too much—on a single occasion or over time—can have serious consequences for our health. Most Americans recognize that drinking too much can lead to accidents and dependence. Alcohol abuse can damage organs, weaken the immune system, and contribute to cancers. Much like smoking, alcohol affects different people differently. Genes, environment, and even diet can play a role in whether you develop an alcohol- related disease.
Moderate or “lower-risk” drinking
People who drink moderately may be less likely to experience an alcohol use disorder (AUD). These drinking levels are:
- For males: No more than 4 drinks on any single day AND no more than 14 drinks per week
- For females: No more than 3 drinks on any single day AND no more than 7 drinks per week
To stay low risk for AUDs, keep within both the single-day and weekly limits. Even within these limits, someone can have problems if they drink too quickly or have other health issues.
To keep risk for problems low:
- Drink slowly
- Eat enough while drinking
|
Certain people should avoid alcohol completely, including those who:
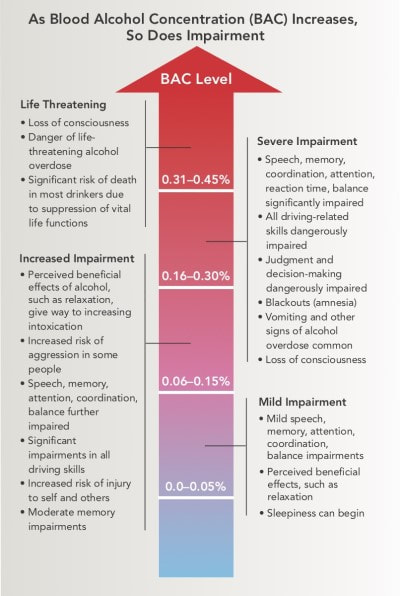
Heavy or “at-risk” drinking For healthy adults in general, heavy drinking means consuming more than the single-day or the weekly amounts listed above. About 1 in 4 people who drink above these levels already has alcohol dependence or alcohol abuse problems. Binge drinking Binge drinking means drinking so much within about 2 hours that blood alcohol concentration (BAC) levels reach 0.08g/dL. For women, this usually occurs after about 4 drinks, and for men, after about 5. Drinking this way can pose health and safety risks, including car crashes and injuries. Over the long term, binge drinking can damage the liver and other organs. |
|
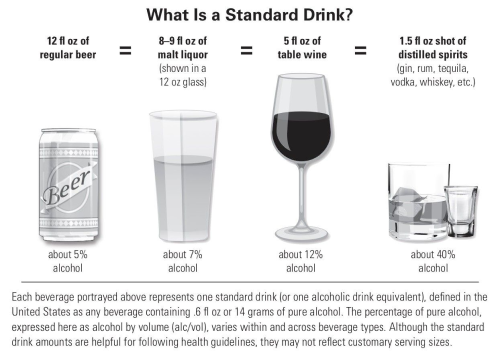
A Little Goes a Long Way: Know the Amounts
Knowing how much alcohol constitutes a “standard” drink can help someone determine how much they are drinking and understand the risks. One standard drink contains about 0.6 fluid ounces or 14 grams of pure alcohol. Examples of one standard drink include:
|
What happens inside the brain?
The brain’s structure is complex. It includes multiple systems that interact to support all of your body’s functions—from thinking to breathing to moving. These multiple brain systems communicate with each other through about a trillion tiny nerve cells called neurons. Neurons in the brain translate information into electrical and chemical signals the brain can understand. They also send messages from the brain to the rest of the body.
Chemicals called neurotransmitters carry messages between the neurons. Neurotransmitters can be very powerful. Depending on the type and the amount of neurotransmitter, these chemicals can either intensify or minimize your body’s responses, your feelings, and your mood. The brain works to balance the neurotransmitters that speed things up with the ones that slow things down to keep your body operating at the right pace. Alcohol can slow the pace of communication between neurotransmitters in the brain.
|
Fetal Alcohol Syndrome
Alcohol can affect the brain at any stage of development—even before birth. Fetal alcohol spectrum disorders are the full range of physical, learning, and behavioral problems, and other birth defects that result from prenatal alcohol exposure. The most serious of these disorders, fetal alcohol syndrome (FAS), is characterized by abnormal facial features and is usually associated with severe reductions in brain function and overall growth. FAS is the leading preventable birth defect associated with mental and behavioral impairment in the United States today. |
The brains of children with FAS are smaller than normal and contain fewer cells, including neurons. These deficiencies result in life-long learning and behavioral problems. Current research is investigating whether the brain function of children and adults with FAS can be improved with complex rehabilitative training, dietary supplements, or medications.
Alcohol and Heart Disease
Americans know how prevalent heart disease is—about 1 in 12 of us suffer from it. What we do not always recognize are the connections heart disease shares with alcohol. On the one hand, researchers have known for centuries that excessive alcohol consumption can damage the heart. Drinking a lot over a long period of time or drinking too much on a single occasion can put someone's heart—and life—at risk. On the other hand, researchers now understand that drinking moderate amounts of alcohol can protect the hearts of some people from the risks of coronary artery disease. Deciding how much, if any, alcohol is right can be complicated. To make the best decision, know the facts and then consult your physician.
Alcohol and Cancer Risk
Genetics, environment, and lifestyle habits can all heighten the risk of getting cancer. We cannot do anything to change our genes, and we often cannot do much to change our environment. But lifestyle habits are a different story.
Drinking too much alcohol is one lifestyle habit that can increase risk of developing certain cancers. This does not mean that anyone who drinks too much will develop cancer. But numerous studies do show the more someone drinks, the more they increase their chances of developing certain types of cancer. The National Cancer Institute identifies alcohol as a risk factor for the following types of cancer:
At least 7 out of 10 people with mouth cancer drink heavily. Drinking five or more drinks per day can also increase risk of developing other types of cancers, including colon or rectal cancer. People who drink are also more likely to smoke, and the combination increases the risk significantly. Smoking alone is a known risk factor for some cancers. But smoking and drinking together intensifies the cancer-causing properties of each substance. The overall effect poses an even greater risk.
The risk of throat and mouth cancers is especially high because alcohol and tobacco both come in direct contact with those areas. Overall, people who drink and smoke are 15 times more likely to develop cancers of the mouth and throat than nondrinkers and nonsmokers. In addition, recent studies estimate that alcohol and tobacco together are responsible for:
Americans know how prevalent heart disease is—about 1 in 12 of us suffer from it. What we do not always recognize are the connections heart disease shares with alcohol. On the one hand, researchers have known for centuries that excessive alcohol consumption can damage the heart. Drinking a lot over a long period of time or drinking too much on a single occasion can put someone's heart—and life—at risk. On the other hand, researchers now understand that drinking moderate amounts of alcohol can protect the hearts of some people from the risks of coronary artery disease. Deciding how much, if any, alcohol is right can be complicated. To make the best decision, know the facts and then consult your physician.
Alcohol and Cancer Risk
Genetics, environment, and lifestyle habits can all heighten the risk of getting cancer. We cannot do anything to change our genes, and we often cannot do much to change our environment. But lifestyle habits are a different story.
Drinking too much alcohol is one lifestyle habit that can increase risk of developing certain cancers. This does not mean that anyone who drinks too much will develop cancer. But numerous studies do show the more someone drinks, the more they increase their chances of developing certain types of cancer. The National Cancer Institute identifies alcohol as a risk factor for the following types of cancer:
- Mouth
- Esophagus
- Pharynx
- Larynx
- Liver
- Breast
At least 7 out of 10 people with mouth cancer drink heavily. Drinking five or more drinks per day can also increase risk of developing other types of cancers, including colon or rectal cancer. People who drink are also more likely to smoke, and the combination increases the risk significantly. Smoking alone is a known risk factor for some cancers. But smoking and drinking together intensifies the cancer-causing properties of each substance. The overall effect poses an even greater risk.
The risk of throat and mouth cancers is especially high because alcohol and tobacco both come in direct contact with those areas. Overall, people who drink and smoke are 15 times more likely to develop cancers of the mouth and throat than nondrinkers and nonsmokers. In addition, recent studies estimate that alcohol and tobacco together are responsible for:
- 80% of throat and mouth cancer in men
- 65% of throat and mouth cancer in women
- 80% of esophageal squamous cell carcinoma, a type of esophagus cancer
- 25 to 30% of all liver cancers
Tobacco
Smoking makes your immune system work overtime. Your body makes white blood cells to respond to injuries, infections, and even cancers. Blood tests show that your white blood cell numbers stay high when you smoke. High numbers mean that your body is constantly fighting against the damage caused by tobacco smoke. This constant stress disrupts how your body works and can lead to disease in almost any part of your body.
Smoking makes your immune system work overtime. Your body makes white blood cells to respond to injuries, infections, and even cancers. Blood tests show that your white blood cell numbers stay high when you smoke. High numbers mean that your body is constantly fighting against the damage caused by tobacco smoke. This constant stress disrupts how your body works and can lead to disease in almost any part of your body.
There is no safe level of exposure to tobacco smoke.
- Any exposure to tobacco smoke – even an occasional cigarette or exposure to secondhand smoke – is harmful.
- You don’t have to be a heavy smoker or a long-time smoker to get a smoking-related disease or have a heart attack or asthma attack that is triggered by tobacco smoke.
- Low levels of smoke exposure, including exposures to secondhand tobacco smoke, lead to a rapid and sharp increase in dysfunction and inflammation of the lining of the blood vessels, which are implicated in heart attacks and stroke.
- Cigarette smoke contains more than 7,000 chemicals and compounds. Hundreds are toxic and at least 69 cause cancer. Tobacco smoke itself is a known human carcinogen.
- Chemicals in tobacco smoke interfere with the functioning of fallopian tubes, increasing risk for adverse pregnancy outcomes such as ectopic pregnancy, miscarriage, and low birth weight. They also damage the DNA in sperm which might reduce fertility and harm fetal development.
Damage from tobacco smoke is immediate.
- The chemicals in tobacco smoke reach your lungs quickly every time you inhale. Your blood then carries the toxins to every organ in your body.
- The chemicals and toxicants in tobacco smoke damage DNA, which can lead to cancer. Nearly one-third of all cancer deaths every year are directly linked to smoking. Smoking causes about 85% of lung cancers in the U.S.
- Exposure to tobacco smoke quickly damages blood vessels throughout the body and makes blood more likely to clot. This damage can cause heart attacks, strokes, and even sudden death.
- The chemicals in tobacco smoke inflame the delicate lining of the lungs and can cause permanent damage that reduces the ability of the lungs to exchange air efficiently and leads to chronic obstructive pulmonary disease (COPD), which includes emphysema and chronic bronchitis.
Smoking longer means more damage.
- Both the risk and the severity of many diseases caused by smoking are directly related to how long the smoker has smoked and the number of cigarettes smoked per day.
- Chemicals in tobacco smoke cause inflammation and cell damage, and can weaken the immune system. The body makes white blood cells to respond to injuries, infections, and cancers. White blood cell counts stay high while smoking continues, meaning the body is constantly fighting against the damage caused by smoking which can lead to disease in almost any part of the body.
- Smoking can cause cancer and weaken your body’s ability to fight cancer. With any cancer – even those not related to tobacco use – smoking can decrease the benefits of chemotherapy and other cancer treatments. Exposure to tobacco smoke can help tumors grow.
- The chemicals in tobacco smoke complicate the regulation of blood sugar levels, exacerbating the health issues resulting from diabetes. Smokers with diabetes have a higher risk of heart and kidney disease, amputation, eye disease causing blindness, nerve damage and poor circulation.
Cigarettes are designed for addiction.
- The design and contents of tobacco products make them more attractive and addictive than ever before. Cigarettes today deliver nicotine more quickly from the lungs to the heart and brain.
- The powerful addicting elements of tobacco products affect multiple types of nicotine receptors in the brain.
- Evidence suggests that psychosocial, biologic, and genetic factors may also play a role in nicotine addiction.
There is no safe cigarette.
- Changing cigarette designs over the last five decades, including filtered, low-tar, and “light” variations, have NOT reduced overall disease risk among smokers and may have hindered prevention and cessation efforts.
- The overall health of the public could be harmed if the introduction of novel tobacco products encourages tobacco use among people who would otherwise be unlikely to use a tobacco product or delays cessation among persons who would otherwise quit using tobacco altogether.
|
|
|
Quitting
Quitting at any age and at any time is beneficial. It is never too late to quit, but the sooner the better. Quitting gives the body a chance to heal the damage caused by smoking. When smokers quit, the risk for a heart attack drops sharply after just 1 year; stroke risk can fall to about the same as a nonsmoker’s after 2-5 years; risks for cancer of the mouth, throat, esophagus, and bladder are cut in half after 5 years; and the risk for dying of lung cancer drops by half after 10 years. Smokers often make several attempts before they are able to quit, but new strategies for cessation, including nicotine replacement and non-nicotine medications, can help.
Tobacco smoke is a toxic mix of more than 7,000 chemicals. Many are poisons. When these chemicals get deep into the body’s tissues, they cause damage. The body must fight to heal the damage each time someone smokes. Over time, the damage can lead to disease.
The chemicals in tobacco smoke reach the lungs quickly and then into the blood. Then the blood flows through arteries carrying the chemicals to tissues in all parts of the body. Lungs, blood vessels, and other delicate tissues become inflamed and damaged.
Damage is Immediate.
The poisons in smoke pose a danger right away. Sudden blood clots, heart attacks, and strokes can be triggered by tobacco smoke. Poisons in tobacco smoke disrupt the way your body heals itself. Even smoking a cigarette now and then is enough to hurt you. Sitting in a smoky bar raises your odds of a heart attack. The more years you smoke, the more you hurt your body. Scientists now know that your disease risk surges even higher after you have smoked for about 20 years. But research shows that if you quit by age 30, your health could become almost as good as a nonsmoker’s. At any age, the sooner you quit, the sooner your body can begin to heal.
Nicotine is powerfully addictive.
Addiction to nicotine changes the chemical balance in your brain. Addiction keeps people smoking even when they want to quit. Breaking addiction is harder for some people than others. Many people need more than one try in order to quit.
Scientists now know more about why the brain craves nicotine. Like heroin or cocaine, nicotine changes the way your brain works and causes you to crave more and more nicotine. These powerful cravings make it hard for you to think about anything else. Smoking can cause both physical and mental addiction.
Cigarettes are designed for addiction.
Cigarette makers have long known that nicotine addiction helps sell their products. Cigarettes today deliver more nicotine and deliver it quicker than ever before. The additives and chemicals that tobacco companies put in cigarettes may have helped make them.
People might have thought that “filtered,” “low-tar,” or “light” cigarettes were less dangerous than others. But research shows that these cigarettes are every bit as addictive and are no safer than other cigarettes. Misleading labels are no longer allowed. Many people who try cigarettes do not know how easy it is to become addicted. Nicotine addiction is so powerful that every day about 1,000 teens become daily smokers. Why is this important? Because most current smokers became addicted as teenagers.
Beating the addiction to tobacco.
Smokers who quit go through withdrawal. The first days are the most uncomfortable. The physical symptoms of nicotine addiction end about 3 weeks after you quit smoking. But you may still have an urge to smoke when you wake up, drink coffee, or are out with friends. It takes longer to break these patterns. But you can beat it.
Tobacco smoke is a toxic mix of more than 7,000 chemicals. Many are poisons. When these chemicals get deep into the body’s tissues, they cause damage. The body must fight to heal the damage each time someone smokes. Over time, the damage can lead to disease.
The chemicals in tobacco smoke reach the lungs quickly and then into the blood. Then the blood flows through arteries carrying the chemicals to tissues in all parts of the body. Lungs, blood vessels, and other delicate tissues become inflamed and damaged.
Damage is Immediate.
The poisons in smoke pose a danger right away. Sudden blood clots, heart attacks, and strokes can be triggered by tobacco smoke. Poisons in tobacco smoke disrupt the way your body heals itself. Even smoking a cigarette now and then is enough to hurt you. Sitting in a smoky bar raises your odds of a heart attack. The more years you smoke, the more you hurt your body. Scientists now know that your disease risk surges even higher after you have smoked for about 20 years. But research shows that if you quit by age 30, your health could become almost as good as a nonsmoker’s. At any age, the sooner you quit, the sooner your body can begin to heal.
Nicotine is powerfully addictive.
Addiction to nicotine changes the chemical balance in your brain. Addiction keeps people smoking even when they want to quit. Breaking addiction is harder for some people than others. Many people need more than one try in order to quit.
Scientists now know more about why the brain craves nicotine. Like heroin or cocaine, nicotine changes the way your brain works and causes you to crave more and more nicotine. These powerful cravings make it hard for you to think about anything else. Smoking can cause both physical and mental addiction.
Cigarettes are designed for addiction.
Cigarette makers have long known that nicotine addiction helps sell their products. Cigarettes today deliver more nicotine and deliver it quicker than ever before. The additives and chemicals that tobacco companies put in cigarettes may have helped make them.
People might have thought that “filtered,” “low-tar,” or “light” cigarettes were less dangerous than others. But research shows that these cigarettes are every bit as addictive and are no safer than other cigarettes. Misleading labels are no longer allowed. Many people who try cigarettes do not know how easy it is to become addicted. Nicotine addiction is so powerful that every day about 1,000 teens become daily smokers. Why is this important? Because most current smokers became addicted as teenagers.
Beating the addiction to tobacco.
Smokers who quit go through withdrawal. The first days are the most uncomfortable. The physical symptoms of nicotine addiction end about 3 weeks after you quit smoking. But you may still have an urge to smoke when you wake up, drink coffee, or are out with friends. It takes longer to break these patterns. But you can beat it.
Interesting reads but not required
- Distribution of Drinks Consumed by U.S. Adults by Average Daily Alcohol Consumption: A Comparison of 2 Nationwide Surveys
- Alcohol Use and Co-Use of Other Substances Among Pregnant Females Aged 12–44 Years — United States, 2015–2018
- Female U.S. high school students more likely to drink alcohol and binge drink than males
- Death Rates from Stroke Among Persons Aged ≥65 Years, by Sex and Age Group — National Vital Statistics System, United States, 2018